 THUNDER BAY – LIVING – Adolescents who live in rural areas and small towns and cities are more likely to abuse prescription painkillers than adolescents who live in large urban areas, according to sociologists.
THUNDER BAY – LIVING – Adolescents who live in rural areas and small towns and cities are more likely to abuse prescription painkillers than adolescents who live in large urban areas, according to sociologists.
Adolescents — youths between 12 and 17 — in rural communities are 35 percent more likely to have abused prescription painkillers in the past year than adolescents living in large cities. Adolescents who live in small cities have a 21 percent greater likelihood of abusing prescription painkillers than their large urban counterparts.
“Over 1.3 million adolescents abused prescription opioids within the last year,” said Shannon Monnat, assistant professor of rural sociology, demography, and sociology, Penn State. “With this number of adolescents there are major implications for increased treatment demand, risk of overdose and even death from these opioids.”
Females are more likely to abuse prescription painkillers than males, according to the researchers.
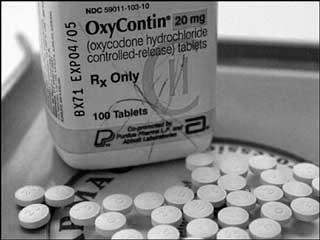
The painkillers that adolescents tend to abuse include OxyContin, oxycodone, Percocet and other morphine-based drugs.
The researchers suggest there are several reasons for this spread of opioid abuse in rural communities, including an increasing number of painkiller prescriptions written for adolescents, as well as the limited types of medical care available in rural areas.
Rural adolescents are more likely to go to emergency rooms for care, rather than to a primary medical practitioner, said Khary K. Rigg, assistant professor of mental health law and policy, University of South Florida, who worked with Monnat. Emergency room doctors are more likely than primary care doctors to prescribe painkillers.
“There has been a shortage of primary care practitioners in rural areas for a long time,” said Monnat. “Often, emergency rooms or urgent care clinics might be the only place for someone to receive treatment in a rural area.”
Rural youths are also less likely to understand the risks of painkiller abuse and less likely to have access to treatment facilities, according to the researchers, who reported their findings in the current issue of the Journal of Rural Health.
Monnat said that rural adolescent painkiller abuse could actually be worse, but several factors often intervene in the youths’ favor. For example, rural youths have less access to illicit drugs, receive more positive forms of peer pressure and report stronger religious beliefs.
“Religious beliefs and the fact that their friends are more disapproving of substance abuse appear to be protective factors against painkiller abuse,” said Monnat.
Painkillers are particularly dangerous because opioid abuse may not be as evident as other forms of substance abuse, such as alcohol.
“Some parents don’t even know their children are addicted to painkillers because their kids are functioning well in everyday life,” said Monnat. “Opioid abuse is different from drinking, for example, because parents can usually tell if their child is drunk, and it’s even different from marijuana use because there are behavioral differences that they may be able to notice if their kid is smoking weed.”
The researchers used data from the 2011 and 2012 National Survey on Drug Use and Health that surveyed 32,036 adolescents on last year prescription opioid misuse.